Pediatric sleep apnea is a sleep disorder that causes children to stop breathing while sleeping. Children are affected by two types of sleep apnea: obstructive sleep apnea and central sleep apnea (central apnea).
Much like adults, children also suffer from sleep apnea with similar if not more consequences than their adult counterparts. Before considering the cure for these children, let’s briefly overview sleep apnea treatment.
Distinguishing Pediatric Sleep Apnea
Pediatric Sleep apnea is of two types. A blockage in the back of the throat or nose causes obstructive sleep apnea. The other type, central apnea, happens when the section of the brain that controls breathing malfunctions. It does not provide regular signals to the breathing muscles to breathe.
The frequency of snoring is one distinction between the two types of apnea. Snoring is common in people with central apnea but more common in people with obstructive sleep apnea. This is because snoring is associated with airway blockage.
Sleep apnea, snoring, or another type of nighttime breathing issue affects between 7% and 11% of youngsters. Approximately 90% of them may go undetected.
Obstructive sleep apnea is far more common in both children and adults than central apnea. It usually begins between the ages of 2 and 8 years old. According to a 2014 study, 1 to 5% of children suffer from obstructive sleep apnea.

Sleep Apnea Symptoms in Children
Aside from snoring differences, the symptoms of obstructive and central apnea may be similar.
Common symptoms of sleep apnea in children include:
- A lot of snoring
- Coughing or choking while sleeping causes breathing interruptions.
- Sleep terrors caused by inhaling through the mouth
- Bedwetting
- Sleeping in unusual positions
However, sleep apnea symptoms do not simply occur at night. If your child experiences a disturbed night’s sleep as a result of this disorder, they may experience exhaustion, difficulty falling asleep, and difficulties getting up in the morning.
Infants and young children with sleep apnea, particularly those with central apnea, may not snort. In this age group, restless or interrupted sleep is sometimes the only indicator of sleep apnea.
Consequences of Untreated Sleep Apnea in Children
Sleep apnea, if left untreated, causes protracted periods of disrupted sleep, resulting in chronic daytime weariness.
A child with untreated sleep apnea may struggle to pay attention at school. This might lead to learning difficulties and low academic performance.
Some children develop hyperactivity, which leads to a misdiagnosis of attention deficit hyperactivity disorder (ADHD). Studies have demonstrated that sleep-disordered breathing can generate symptoms comparable to those seen in ADHD and that treating sleep apnea, if present, can significantly reduce these symptoms.
Untreated sleep apnea causes growth delays, cognitive disabilities, and heart difficulties in more severe cases. Children with untreated sleep apnea may struggle socially as well. These consequences are likely to improve if sleep apnea is adequately treated.
Untreated sleep apnea can also lead to excessive blood pressure, putting people at risk of stroke and heart attack. It may also be linked to childhood obesity.
Diagnosing Sleep Apnea in Children
If you suspect your child has sleep apnea, consult a doctor. Your pediatrician may recommend a sleep specialist.
The doctor will ask about your child’s symptoms, perform a physical examination, and, if necessary, schedule a sleep study to diagnose sleep apnea correctly.
Sleep research
Your youngster will spend the night in a hospital or sleep clinic for the sleep study. A sleep technician wears test sensor and measures the following parameters during the night:
- Breathing patterns and brain wave activity
- Oxygen saturation, heart rate, muscle activity
Electrocardiogram (ECG or EKG)
If your child’s doctor suspects that he or she has a heart condition, an electrocardiogram (ECG or EKG) may be scheduled in addition to the sleep study. The electrical activity in your child’s heart is recorded throughout this test.
Note: Consult a doctor if your child matches the criteria for sleep apnea and exhibits hyperactivity or indicators of behavioral issues.
Treating Sleep Apnea in Children
There are no standardized criteria for treating pediatric sleep apnea. A doctor may choose not to treat mild sleep apnea without symptoms, at least not straight away.
Some children outgrow sleep apnea, so their doctor may keep an eye on their condition to see if it improves. They must balance the advantages of doing so against the potential of long-term problems from untreated sleep apnea.
Initial therapies for children with obstructive sleep apnea include diet and surgery. Initial therapies for children with central apnea include diet and treatment of underlying problems. Other options include;
Changes in Lifestyle
Your child’s doctor may recommend physical activity and diet to address sleep apnea if he or she is obese.
Surgery
When swollen tonsils or adenoids cause obstructive sleep apnea, both the tonsils and adenoids are usually removed surgically to open up your child’s airway.
According to a 2016 study, adenoid removal was just as beneficial as tonsil and adenoid removal for a child who was under the age of seven, did not have childhood obesity, had moderate, rather than severe, obstructive sleep apnea, and had tiny tonsils.
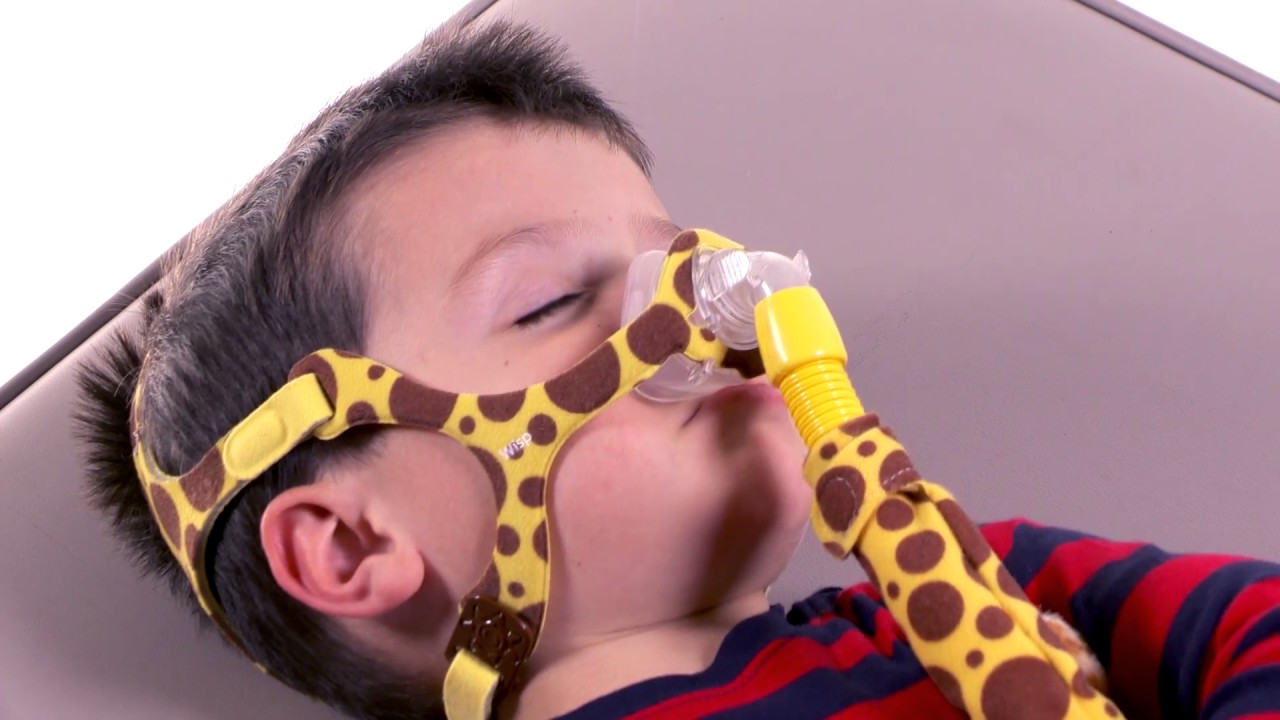
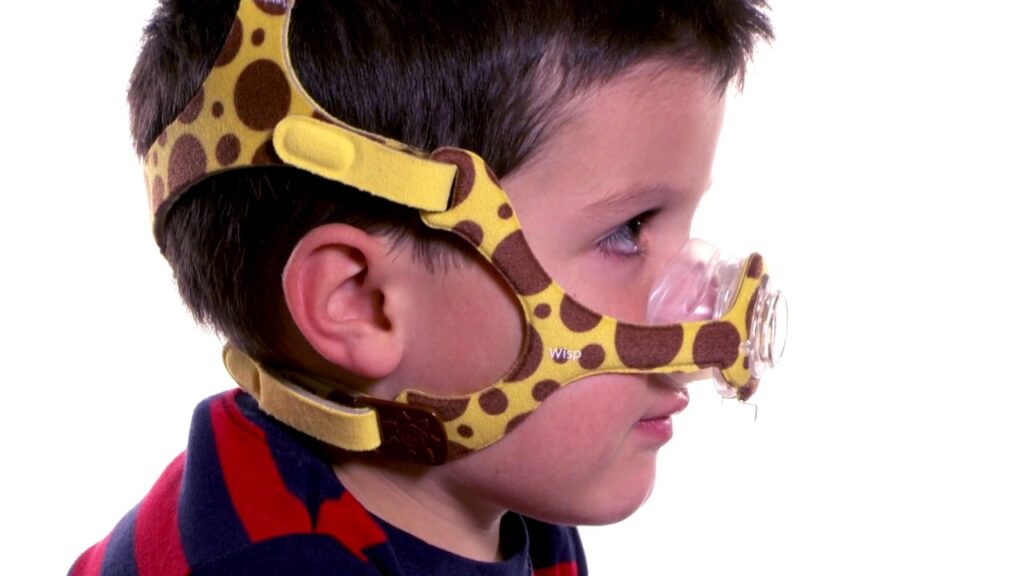
CPAP (Continuous Positive Airway Pressure) Therapy
Your child may require continuous positive airway pressure (CPAP) therapy if his or her sleep apnea is severe or does not improve with initial treatment.
CPAP therapy involves your child sleeping with a mask that covers their nose and mouth. The mask is linked to a CPAP machine, which supplies a constant flow of air to keep their airway open. CPAP can alleviate the symptoms of obstructive sleep apnea but cannot cure it.
Mouth Appliances
Oral appliances are also available for children with obstructive sleep apnea to wear while sleeping. These devices are intended to hold the jaw forward, maintain the tongue in place, and keep the airway open. CPAP is generally more effective, but youngsters tolerate oral appliances better and are more likely to use them every night.
Oral appliances do not benefit every child, but they may be an option for older children who have stopped growing facial bones.
Device for Noninvasive Positive Pressure Ventilation (NIPPV)
A noninvasive positive pressure ventilation device (NIPPV) may be more effective for children with central apnea. These gadgets allow you to program a backup breathing rate. This ensures that a youngster takes a certain number of breaths every minute, even if the brain does not send a signal to do so.
Apnea Detectors
Infants with central apnea can benefit from apnea alarms. When an apnea episode occurs, the alarm goes off. This awakens the infant and brings the apneic episode to an end. If the infant outgrows sleep apnea, you can turn off the alert. Outside of a hospital environment, apnea alarms are almost never suggested.
Other resources:
Side effects of CPAP masks therapy
How Resmed Airsense 10 CPAP Machine Can Help Treat Your Sleep Apnea Symptoms
How to Avoid Rainout, Water, and Moisture in Tubing And Masks of Your CPAP Machine