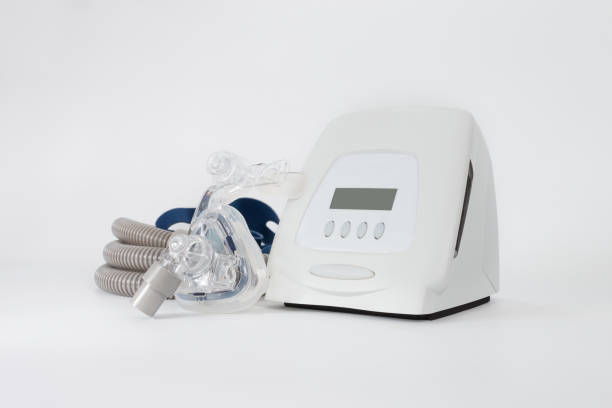
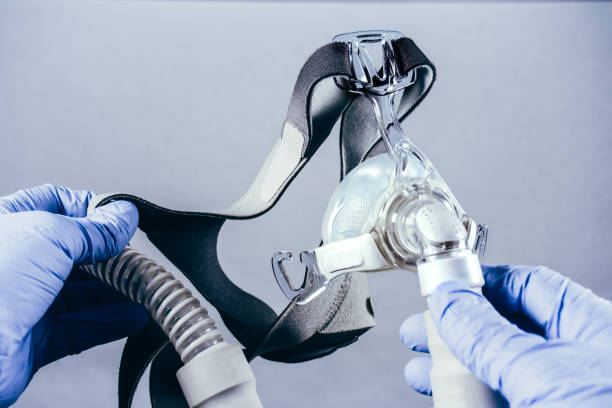
Although it has a few potential negative effects, continuous positive airway pressure (CPAP), which is used to treat obstructive sleep apnea, is generally safe. The most frequent complaints are related to air pressure or discomfort from the mask itself, and these problems may often be resolved by adjusting your machine’s settings or your mask’s fit.
Don’t make these modifications on your own since CPAP is a prescription treatment with many factors to take into account or you might encounter negative consequences.
Related: Read this before getting those CPAP masks
CPAP Masks Leaking Air
Air leaks are by far the most typical CPAP-related complaint. Air may leak around the edges of the CPAP masks if it does not fit snugly, particularly if you change positions while you sleep.
Leaks are more likely to occur with larger CPAP masks, such as those that cover the mouth and nose. Leaks might hinder your treatment by decreasing the amount of pressure applied, or they could be loud and wake up your bed mate.
By utilizing a nasal mask or nasal cushions, air leakage may be minimized. Changing the pressure settings for your CPAP masks might sometimes assist if the fit is a problem for you.
If there is too much air pressure, the extra air leaks out of the mouth or around the edges of the mask. Before making any changes, talk this over with your doctor.
Skin rashes or marks
If your CPAP masks doesn’t fit correctly, it might leave markings on your skin and cause sores or even ulcers, particularly around the bridge of your nose. A rash or skin irritation may also occur in those with sensitive skin, particularly when latex-containing CPAP masks are used.
These symptoms may be alleviated by mask liners, barrier lotions, relaxing the mask, or a better-fitting mask.
Dryness of the Mouth or Nose
Leakage is often accompanied by dryness in the mouth or nose. This might cause nosebleeds or possibly harm to your teeth and gums. A parched mouth or tongue might result from opening your mouth wide.
An over-the-counter nasal saline spray might assist if your nose is dry.
You may avoid drying out by using heated humidifiers and heated tubing. You may use a chinstrap or a full-face mask that covers your nose and mouth to prevent your mouth from opening.
Difficulty in exhaling
When you first begin utilizing CPAP treatment, you could find it challenging to breathe out against the pressure even when it is simple to breathe in. Over time, this could get better, but the effort can also keep you up at night.
It may be beneficial in certain circumstances to ramp up from a lower starting pressure or include a function that makes exhaling simpler. It could be required to lower all pressures. Bi-level treatment, which involves breathing in at one pressure and exhaling at a lower pressure, may be necessary in rare circumstances.
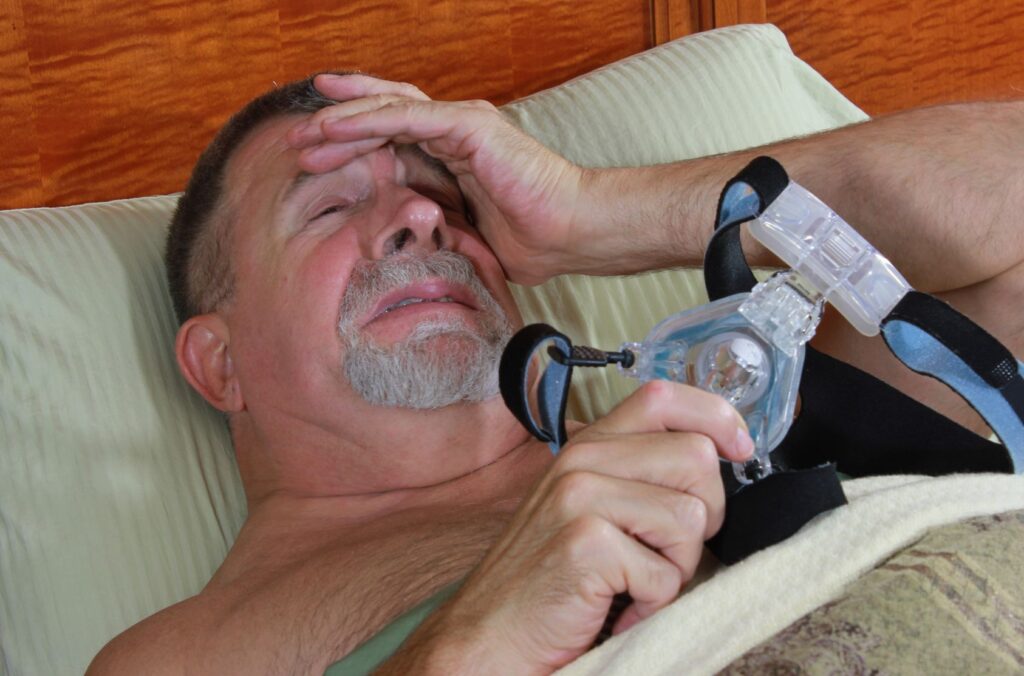
Swallowing Air
Aerophagia, the act of ingesting air, is common (literally “air eating”). Aerophagia may be to blame if you wake up with air in your stomach.
Among the signs are: bloating, farting, and burping.
Swallowing air may indicate excessive CPAP pressures. The extra air may enter your stomach via your esophagus rather than your upper airway.
Reduced pressures might aid in avoiding this. The usage of wedge pillows when sleeping, GERD and heartburn drugs, and bi-level therapy are further therapies for aerophagia.
The emergence of central sleep apnea
Some persons may begin to have bouts of the breath holding associated with central sleep apnea after beginning CPAP treatment. If central apneas did not account for the bulk of your breathing disruptions before to commencing CPAP but now account for more than five occurrences per hour, you may have complicated sleep apnea. 4
Sometimes, this goes away with time, and it could be treated by by reducing the CPAP pressure. Adaptive servo-ventilation (ASV) therapy, in which the air volume and speed may be adjusted to vary based on your demands, may sometimes be necessary as a change in treatment.
Facial growth issues in children
Children who use CPAP should be closely watched to prevent midface development issues brought on by the pressure of the mask over the nose.
Nasal cushions and other modern mask designs may lessen this danger.
Claustrophobia
When wearing a mask, some individuals feel constrained or contained. If you take the time to gradually become used to wearing the mask, this usually gets better with time.
Talk to your healthcare professional about claustrophobia remedies if you have difficulty using your CPAP masks due to claustrophobia.
Loud Sound
For the person you sleep with in particular, the noise might be disruptive to sleep. Even though the technology being utilized now is far quieter than it was in the past, it can take some getting used to. Overall, snoring, which is highly frequent with obstructive sleep apnea, is more difficult for spouses to get used to than the predictable sounds of CPAP.
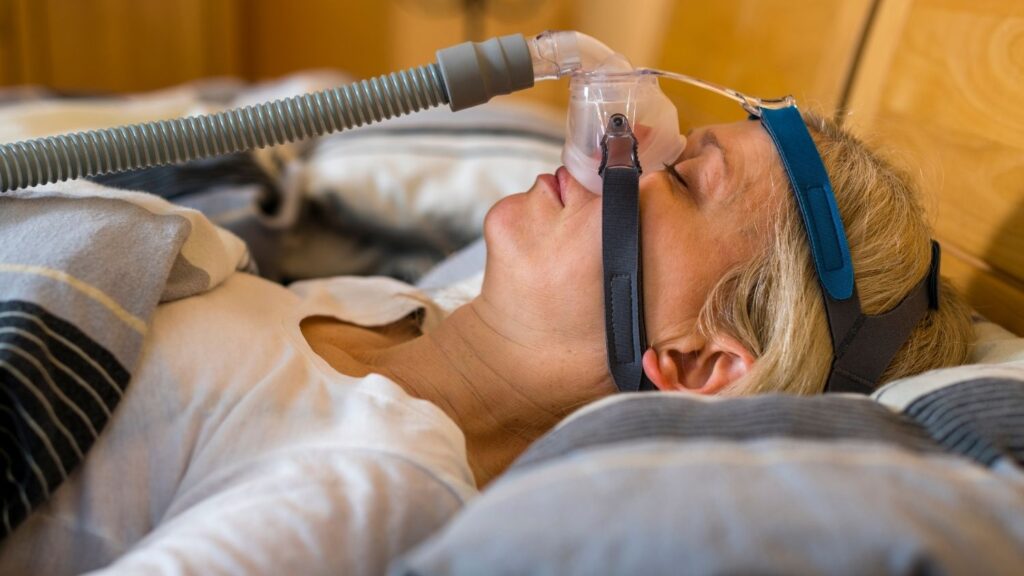
Sex Drive
Some individuals may object that wearing CPAP masks is uncomfortable and could reduce sex desire in one or both partners. If this is a problem, it is important to openly discuss it with your spouse in order to determine when you will wear it and how to prevent having bad sentiments about the CPAP masks.
Changing the CPAP setting
The CPAP machine’s pressure settings may sometimes need to be changed if your obstructive sleep apnea risk factors change. This may be essential for a number of reasons, including:
Weight fluctuations:
Losing weight may cause issues with air swallowing, mask leaks, or difficulty breathing out against the pressure. Being overweight increases your chance of developing sleep apnea. It could help to reduce your CPAP pressure. A modification in CPAP pressure may also be necessary due to weight increase.
Allergies:
If you suffer from environmental allergies, effective therapy with drugs or nasal sprays may be able to lower your need for pressure by enhancing nasal airflow.
Surgical procedures:
You may need different amounts of CPAP treatment after having a tonsillectomy, a nasal septoplasty, or soft palate or tongue surgery.
Substance abuse:
Smoking may make sleep apnea and snoring worse. Alcohol use just before night might relax your muscles and make your obstructive sleep apnea symptoms worse. Your pressure requirements can decrease if you stop using any of these drugs.
Medication:
Drugs like benzodiazepines and muscle relaxants may make your symptoms worse. If you stop using them, your need for pressure can decrease.
Keep in mind that your settings should be adjusted by your healthcare practitioner. Making the decision on your own might be risky.